Department of Otolaryngology—Head & Neck Surgery

NYU Langone Health’s Department of Otolaryngology—Head and Neck Surgery delivers excellence and innovation in diagnosing, managing, and treating ear, nose, and throat disorders and providing medical and surgical care for acquired and congenital head and neck conditions. We are proud to have performed the first pediatric auditory brainstem implantation in the United States in 2012, and remain the only hospital in the region to offer the procedure for patients with neurofibromatosis type 2.
We offer otolaryngology—head and neck surgery educational programs for medical students, residents, fellows, and graduate and postdoctoral students. Our faculty are committed to training the next generation of specialists and driving new standards of patient care through basic science, translational, and clinical otolaryngology—head and neck surgery research in the following areas:
- audiology
- cochlear and auditory brainstem implantation
- facial plastic and reconstructive surgery
- general otolaryngology and sleep surgery
- head and neck surgery
- laryngology
- pediatric otolaryngology
- otology, neurotology, and skull base surgery
- rhinology and endoscopic skull base surgery
We draw upon the expertise of specialists across our academic medical center, including at our nationally recognized Cochlear Implant Center, the Comprehensive Neurofibromatosis Center, the Voice Center, and the Pediatric Aerodigestive Center, part of Hassenfeld Children’s Hospital at NYU Langone, to achieve new standards of excellence.
cochlear implant surgeries performed each year
clinical trials in head and neck cancer, otology and neurotology, laryngology, and pediatric otolaryngology
active grants from the National Institutes of Health

Make a Gift

Related News

Advancing Minimally Invasive Head & Neck Cancer Treatments
Brain Circuit Explains Why Infant Cries Prompt Milk Release
Jaw Surgery Helps Long Island Baby Breathe More Easily

Renowned Head & Neck Surgeon Named Chair of Otolaryngology

This Mom Had Brain Surgery & Ran a Marathon 18 Months Later
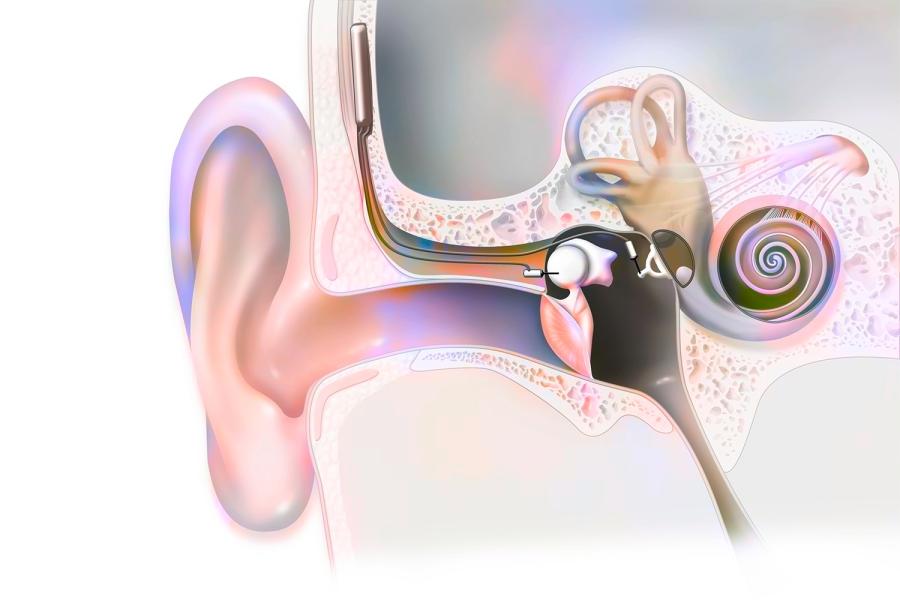
Neuroplasticity May Speed Up Adjustment to Cochlear Implants

Baby Survives CHAOS After High-Risk, Complex Procedure

Surgeon Discusses Treatment Advances for Head & Neck Cancer

Head & Neck Cancer Doctors Help People Look Better

Ambitious Surgery Plan Helps Musician Regain Partial Hearing

New Hearing Loss Program Launches for Immigrant Families